

What Are The Red Flags Of Rheumatoid Arthritis?
Table of Contents
Rheumatoid arthritis is a chronic inflammatory disorder affecting more than just joints. In some people, the disease damage a wide range of body systems, including the heart, skin, eyes, lungs, and blood vessels. Rheumatoid arthritis occurs when the immune system mistakenly attacks the body’s tissues, known as autoimmune disease.
Unlike the wear and tear damage caused by osteoarthritis, rheumatoid arthritis impresses the lining of joints, causing painful swelling that can eventually lead to bone erosion and joint deformity. The inflammation linked with rheumatoid arthritis can damage other parts of the body. While new drugs have dramatically improved treatment options, severe rheumatoid arthritis can still be physically disabling.
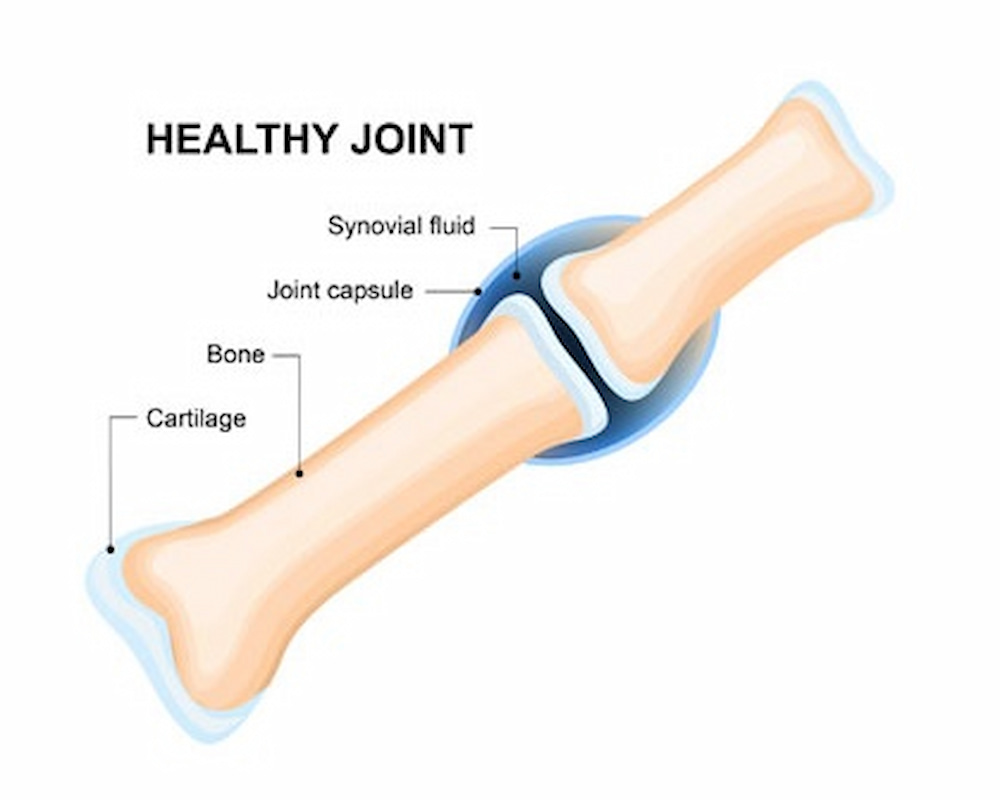
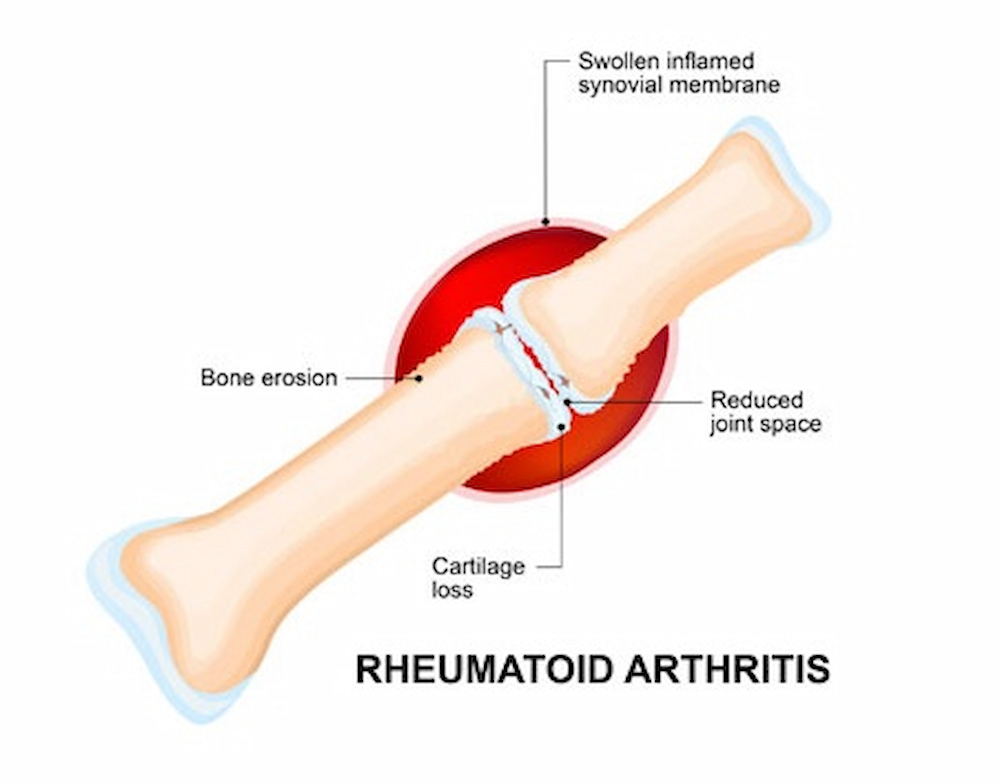
What is rheumatoid arthritis, and how does it happen?
Rheumatoid arthritis (RA) is a chronic inflammatory disease that causes joint pain, edema, and stiffness (decreased flexibility). This disease is one of the different types of arthritis and occurs when the body’s immune system mistakenly attacks our joints and causes their destruction and inflammation. The exact cause of RA and why the immune system attacks the joints is unknown.
Rheumatoid arthritis primarily affects our joints, but it can affect many other parts of the body, in addition to the joints.
It should be remembered that rheumatoid arthritis differs from osteoarthritis, the most common form of arthritis. Osteoarthritis happens when the cartilage that supports the joints wears down over time. However, a person may have both of these disorders simultaneously.
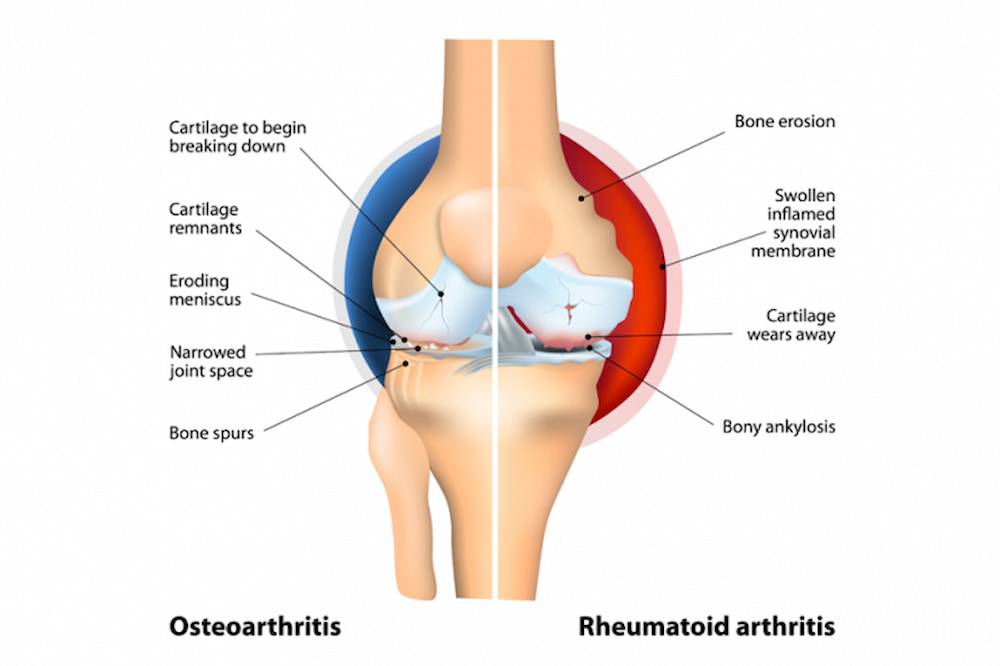
RA halmark symptoms develop gradually. Many sufferers have persistent symptoms, others that resolve entirely, and others have intermittent periods of symptoms and no symptoms. The onset time, severity of the disease, symptoms, and complications of this disease can be very different from one person to another.
Rheumatoid arthritis occurs when the immune system mistakenly attacks your body tissues. Unlike the wear and tear injury of osteoarthritis, rheumatoid arthritis impacts the lining of joints, causing painful edema that can lead to bone erosion and joint deformity.
The inflammation linked with rheumatoid arthritis can damage other parts of the body. While new types of drugs have dramatically improved treatment options, severe rheumatoid arthritis can still be physically disabling.

What are the four stages of rheumatoid arthritis?
There are four distinct stages of rheumatoid arthritis (RA) that can progress over time, although not all patients experience all stages the same way. Factors such as how a person and their doctor manage rheumatoid arthritis, how doctors initially diagnose and start treatment, and several lifestyle or genetic factors also help determine how the disease progresses.
The four stages of RA are:
- Stage 1: Early RA
- Stage 2 or moderate RA
- In stage 3 or severe RA
- Stage 4, or the final stage of RA
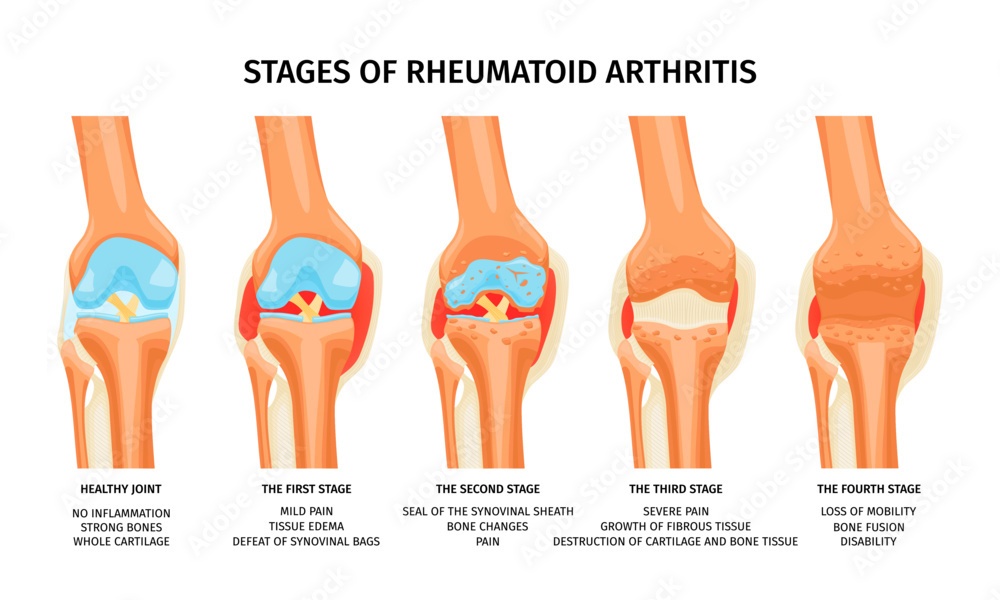
Regardless of the stage, RA halmark symptoms affect both sides of the body equally and are often worse when a person first stands up or after a long period of immobility. Ultimately, rheumatoid arthritis symptoms stem from joint inflammation in a person’s joints and affect the tissues that cover them, called synovial tissues.
Furthermore, as RA progresses and symptoms worsen, this chronic inflammation causes joint damage, affecting more joints and resulting in other complications such as dysfunction and limited mobility.
A person can manage all stages of rheumatoid arthritis using a combination of medications, lifestyle or habit changes, over-the-counter (OTC) medications, and home remedies.
Stage 1 of rheumatoid arthritis
Stage 1 is the initial stage of RA. Many people feel joint pain, stiffness, or inflammation at this stage. In stage 1, there is inflammation inside the joint. The joint tissue becomes swollen. No damage is done to the bones, but the joint’s lining, the synovium, will inflame. People with stage 1 RA, or early RA, often experience inflammation of the joint tissue, which causes the following symptoms:
- swelling
- joint’s pain
- hardness, hardness
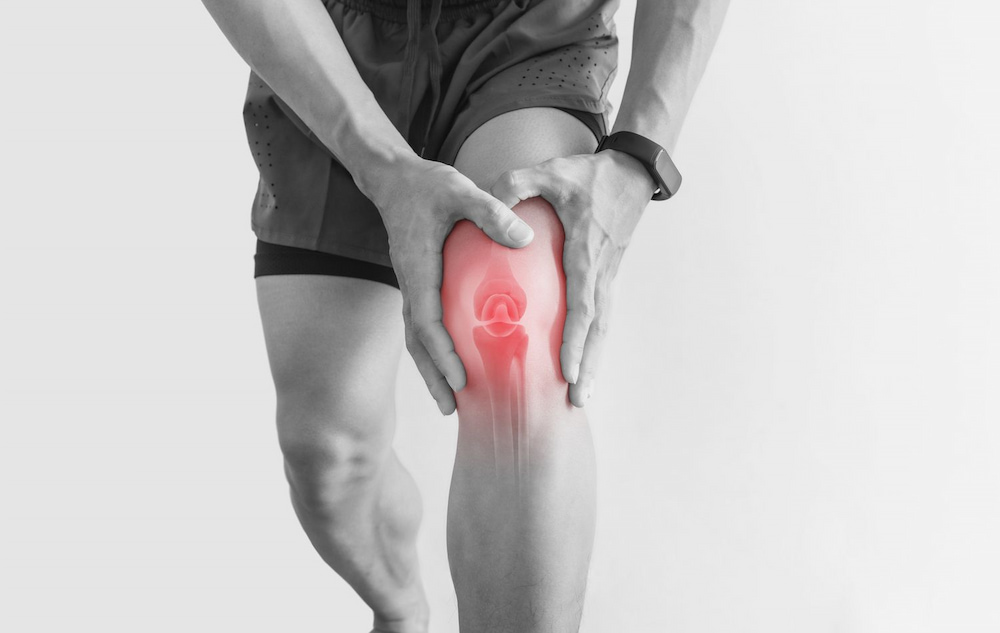
Stage 2 of rheumatoid arthritis
Stage 2 is the intermediate stage of RA. At this stage, inflammation of the synovium causes damage to the joint cartilage. Cartilage is the texture that covers the ends of bones at joints. When cartilage is damaged, people may experience pain and reduced mobility. Even the range of motion in the joints may be limited.
People with stage 2 RA, or moderate rheumatoid arthritis, often experience more severe or extended periods of stage one symptoms and increasingly frequent or prolonged periods of reduced mobility or range of motion. In stage 2 RA, synovial inflammation in the joints can begin to damage the joint cartilage.
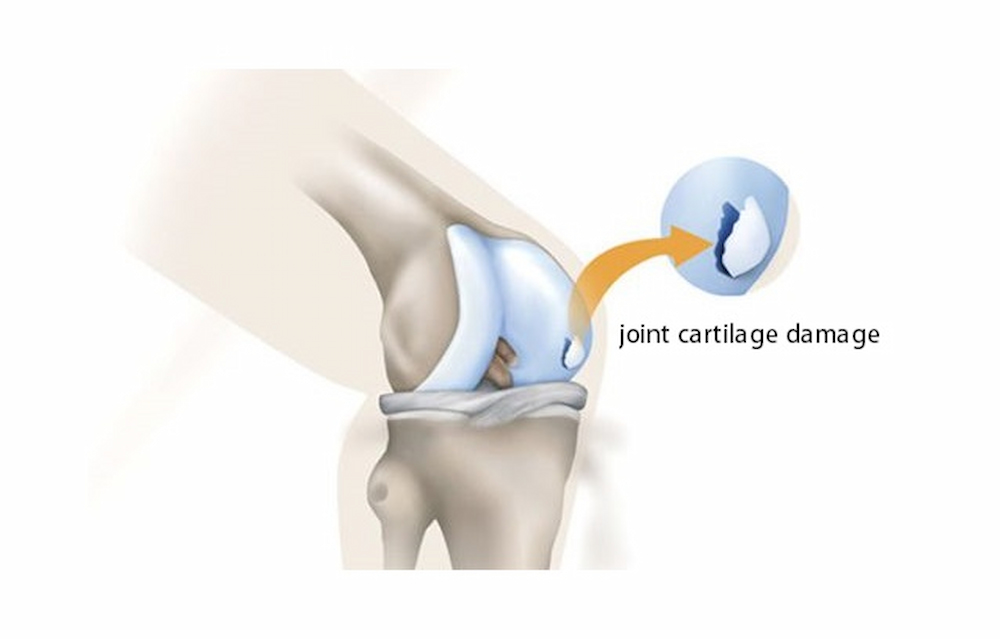
Stage 3 of rheumatoid arthritis
When RA progresses to stage 3, it is considered severe. At this stage, the damage extends not only to the cartilage but also to the bones themselves. As the cushion between the bones wears down, they rub against each other. Pain and swelling are more likely in these conditions. Some people may experience more muscle weakness and reduced mobility. The bone may become damaged (erosion), and some deformities may occur.
People with stage 3 RA, or severe rheumatoid arthritis, often experience much more severe pain, frequent joint swelling, and related symptoms than those with stage 1 or 2 RA. In stage 3 RA, the inflammation becomes so severe that it destroys the bones and cartilage of the joint. Other worst symptoms of stage 3 RA include:
- Further reduction in range of motion
- Physical abnormalities of the joints, such as bent or impinged hands and toes
- Formation of rheumatoid nodules around the joints
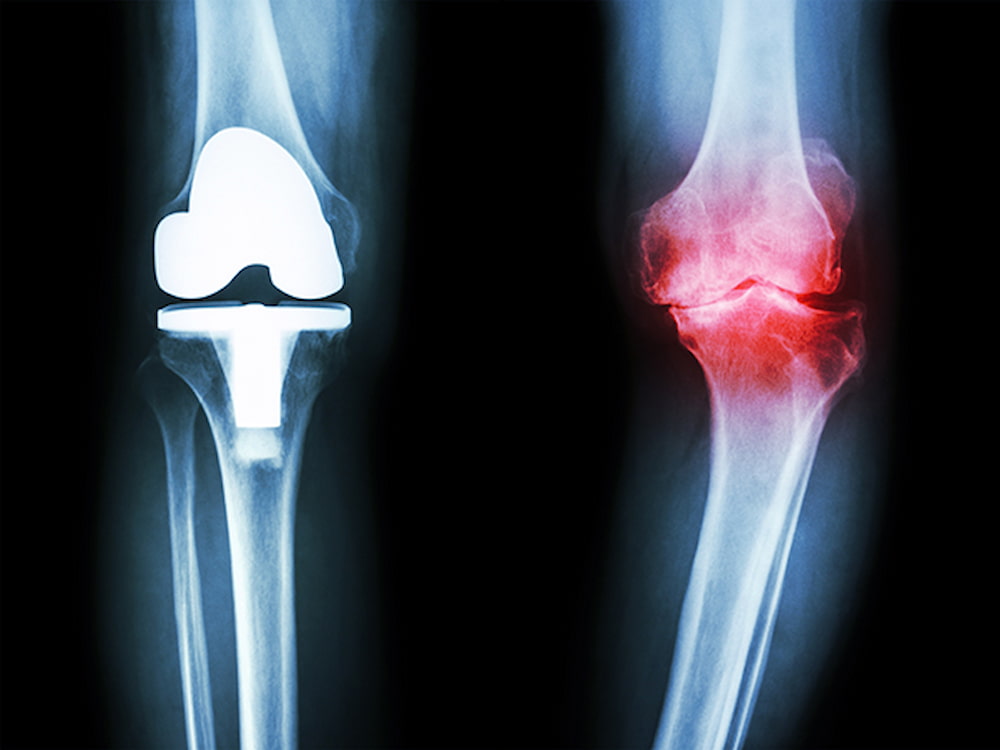
Stage 4 of rheumatoid arthritis
In stage 4, there is no more inflammation in the joint. This is the final stage of RA when the joints no longer work. In late-stage RA, people may still experience pain, swelling, stiffness, loss of mobility, and decreased muscle strength. Joints may disappear, and bones may fuse (ankylosis). Progressing through all four stages can take years; some people experience only some stages in their lifetime. Some people do not have periods of RA progression. In some cases, this may mean that the RA is in remission.
In this last stage, the end stage of RA, the inflammation of the joint tissue is significantly reduced. Also, this condition further compromises the joint’s normal function. Most people with end-stage RA experience the same symptoms as people with early-stage RA, although functional capacity symptoms are more severe, chronic, and debilitating.
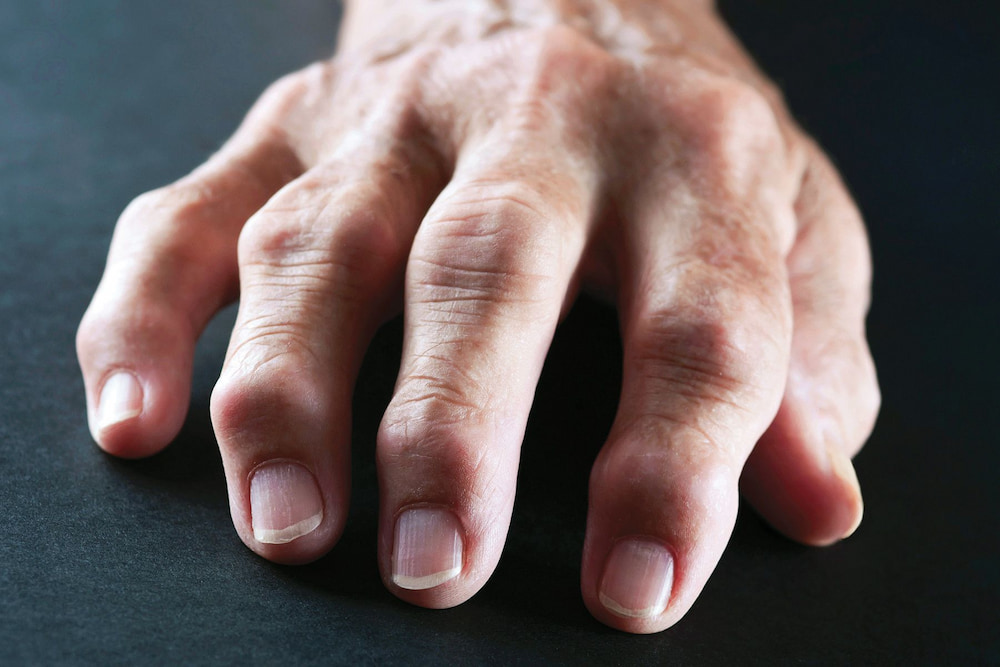
What are usually the first signs of rheumatoid arthritis?
Usually, the first signs and halmark symptoms of rheumatoid arthritis may include:
*Sensitive, hot, and swollen joints
*Stiffness of the joints, which usually worsens in the morning and after inactivity
Fatigue, fever, and loss of appetite
Related: “What Is The Difference Between Intermittent, Remittent, And Relapsing Fever?“
Early rheumatoid arthritis first affects your smaller joints, especially the joints that connect fingers to your hands and your toes to your feet. As the disease progresses, symptoms often include the wrists, knees, Elbows, ankles, hips, and shoulders being extended. In most cases, symptoms happen in the same joints on both sides. About 40 percent of patients with rheumatoid arthritis(RA) also experience signs and symptoms that do not involve the joints. Areas that may be affected include:
- heart, skin, eyes, lungs, kidneys, salivary glands, nervous tissue, bone marrow, blood vessels

What are the red flags of rheumatoid arthritis?
Rheumatoid arthritis signs and symptoms may change in severity and may even be periodic and change. Rheumatoid arthritis can change the form of the joints and dislocate them.
Although joint involvement is the most common symptom of rheumatoid arthritis, this disorder may also cause various other problems. These red flags of rheumatoid arthritis can be caused by inflammation, side effects of drugs used to treat the disease (for example, steroids), or a combination of different factors.
The red flags of rheumatoid arthritis include decreased bone density, muscle weakness, fatigue, skin problems, eye problems (including inflammation, redness and eye pain, and vision problems), lung inflammation which may cause shortness of breath and dry cough, inflammation, Blood vessels and pericarditis (inflammation of the membrane covering the heart).

The most common red flags of rheumatoid arthritis are:
- Swelling, pain, and heat in the joints. Smaller joints of the hands or feet are usually affected.
- Morning stiffness and stiffness lasting more than 30 minutes (or joint stiffness lasting more than 30 minutes if resting during the day).
- Decreased joint range of motion and muscle strength
- Chronic weakness and fatigue
- Abnormal sensations such as burning or shooting
- Difficulty sleeping due to pain
- muscle weakness
- Flu-like symptoms, such as feeling hot and sweating
- Headache
- Neck Pain
- loss of appetite
- Fever
Conclusion
The cause of rheumatoid arthritis(RA) is the immune system attacking the inner layer of the joint membrane or synovial membrane (the layer of membranes around the joint). The usual role of the immune system is to protect us against infections.
Rheumatoid arthritis has a symmetrical pattern; Therefore, joints on both sides of the body are affected by rheumatism. If the right wrist is injured, the symptoms will also appear in the left wrist.
It is worth mentioning that the symptoms of joint rheumatism appear differently in each patient. The course and severity of the disease vary from person to person, and no two diseases are alike. Symptoms can change daily, and there are times when the disease is active and sometimes inactive and silent.
Symptoms may come and go or last for several years. The patient may have only a few of the above symptoms or other than those listed.



2 Responses
How can we find out bone density at home? And how can we find out that we have rheumatoid arthritis through bone density?
Bone density cannot be determined at home, but you need an imaging test in a laboratory environment.
Bone densitometry is a non-invasive imaging test commonly used to measure bone density. This test involves using X-ray technology to measure the amount of calcium in your bones. It can detect osteoporosis, which is a condition that makes bones weak and brittle, increasing the risk of fracture.
Bone densitometry can be performed in a medical setting, such as a radiology clinic or a hospital. However, it requires specialized equipment and trained personnel to operate and interpret the results.
Rheumatoid arthritis (RA) is typically diagnosed by a combination of medical history, physical examination, and laboratory tests, including blood tests and imaging studies. The diagnosis is made by a physician who specializes in rheumatology, who can also evaluate the extent of joint damage using X-rays, magnetic resonance imaging (MRI), or ultrasound.
Bone density testing can help determine the extent of bone loss associated with RA and can be used to assess the severity of the disease and monitor response to treatment. It is important to note that while bone density testing can provide information about the health of your bones, it does not diagnose RA or any other condition. A combination of clinical judgment, laboratory results, and imaging studies is needed to diagnose and manage RA accurately.