

Insulin Function In Diabetes. Is It An Effective Treatment?
Insulin is a hormone in your pancreas, the gland behind your stomach. This gland allows your body to use glucose for energy. Glucose is a type of sugar found in many carbohydrates.
After eating food, the digestive system breaks down carbohydrates and changes them into glucose. Glucose is then absorbed through the wall of the small intestine into your bloodstream. When glucose enters your bloodstream, insulin function causes glucose to be absorbed throughout your body, and cells use it for energy.
This hormone also helps balance your blood glucose levels. When too much glucose is in your blood, insulin signals your body to store the excess in the liver. Stored glucose is released when your blood glucose levels are low, such as between meals or when your body is stressed or needs an energy boost.
Table of Contents
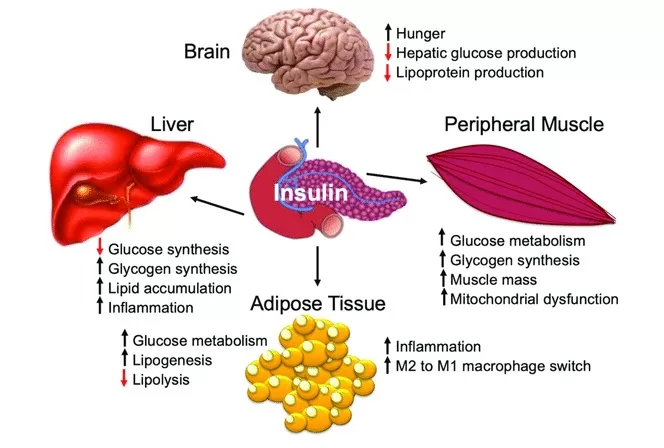
Understanding diabetes and using insulin function
Diabetes occurs when your body does not use or make enough insulin properly. There are two main types of diabetes: type 1 and type 2.
Type 1 diabetes
Type 1 diabetes is an autoimmune disease. It is a disease that causes the body to attack itself. If you have type 1 diabetes, your body cannot produce this hormone. This is because your immune system has destroyed all the cells in your pancreas that produce this hormone. The disease is often diagnosed in young people but can also develop in adulthood.
Type 2 diabetes
In type 2 diabetes, your body becomes resistant to the effects of insulin. This means that your body needs more insulin to have the same effects. Therefore, your body overproduces this hormone to keep blood glucose levels average. ( In regard to blood the article “How To Increase Blood Pressure?” would be beneficial ) However, after several years of excessive production of this hormone in the body, the cells that produce this hormone in the body are destroyed. Type 2 diabetes affects people of any age but generally occurs in old age.
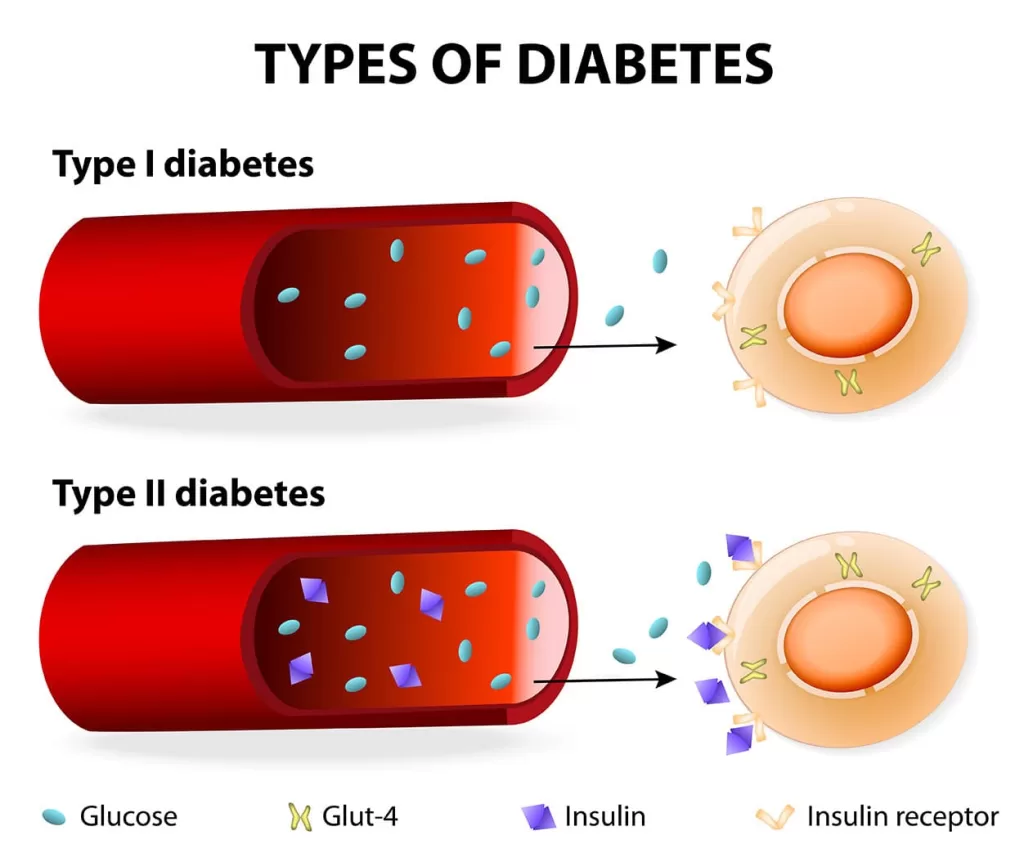
insulin function as a treatment for diabetes
Injection of this hormone can cure both types of diabetes. This hormone is injected as a replacement for your body’s insulin or as a supplement. People with type 1 diabetes cannot make this hormone, so they may need insulin to control their blood glucose levels.
Many people with type 2 diabetes can manage their blood glucose levels with lifestyle changes and oral medications. However, if these treatments do not help control glucose levels, people may need this hormone to control their blood glucose levels.
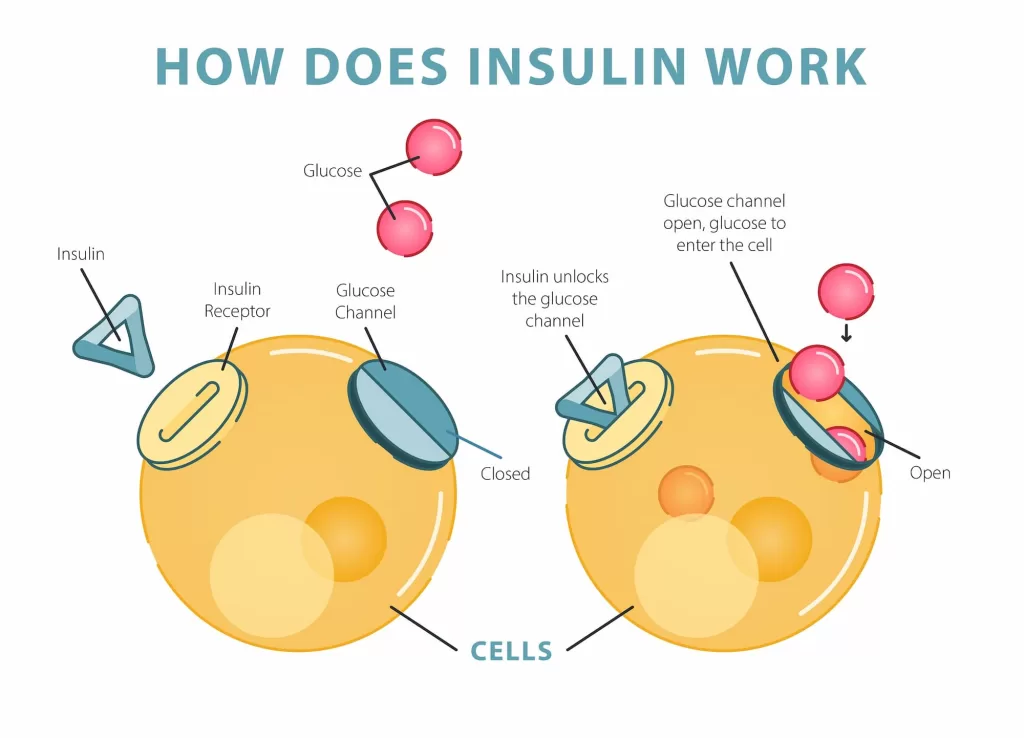
Types of insulin function therapy
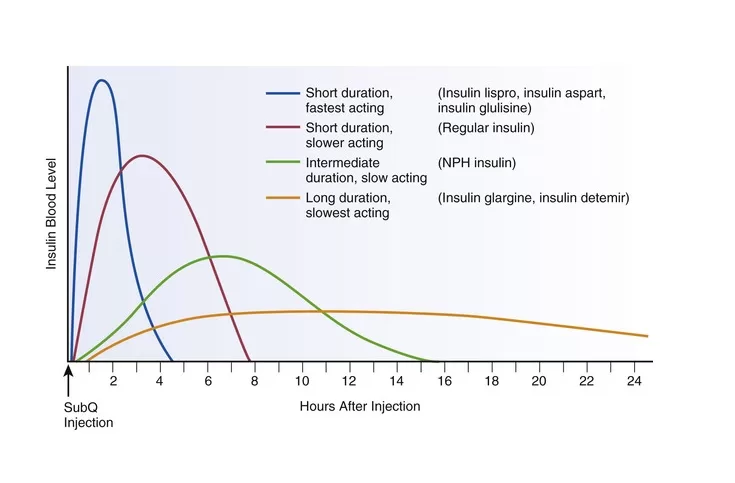
All types of insulin produce a similar effect. They do the same natural increase or decrease of insulin in the body during the day. Different combinations of insulin affect the speed and duration of their effect.
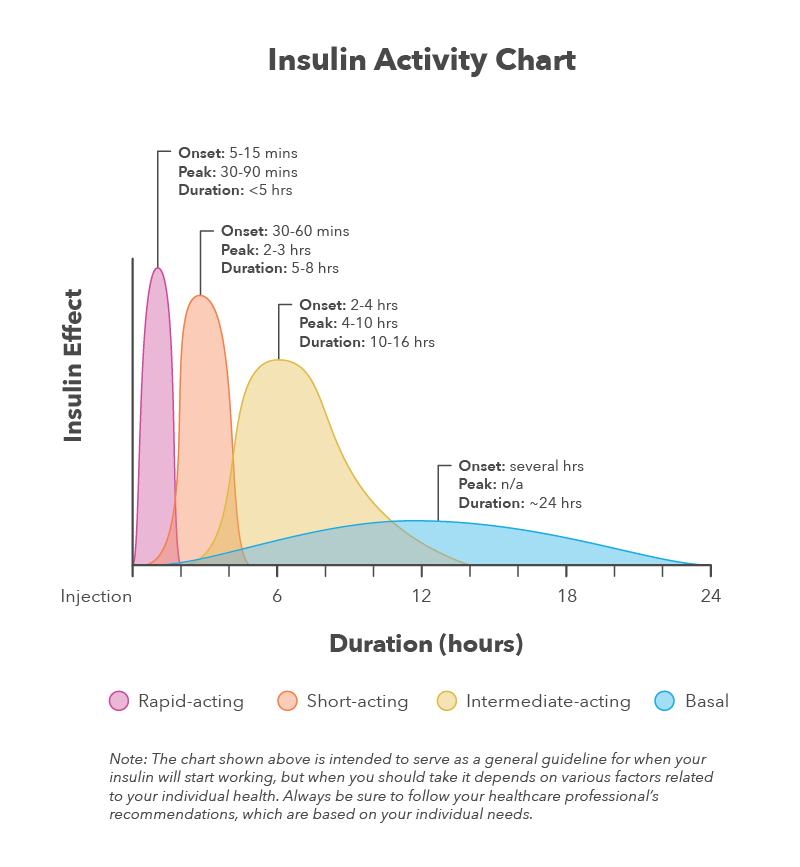
Insulin function with immediate effect: this type of hormone begins to work approximately 15 minutes after injection. The effects of this type of insulin can last between three and four hours. This type of hormone is often used before meals.
Insulin function with short-term effect: this hormone is injected before meals. Its effectiveness lasts 30 to 60 minutes after injection and lasts five to eight hours.
Intermediate-acting insulin function: This type of hormone starts working 1-2 hours after injection, and its effects may last 14-16 hours.
Insulin function with long-term effect: this type of insulin may not have an effect until about 2 hours after injection; this type lasts up to 24 hours.
The most common types of insulin are NPH and regular insulin. These two types of insulin are different in terms of the time of onset, maximum, and termination of effect.
New types of insulin
Although some types of oral insulin are being tested at research levels and sometimes at a limited level in a few volunteers, they have yet to be available for daily use in treating general patients. For example, inhalation and oral insulin functions are studied in research centers. However, they have yet to enter the consumer market, or after entering it in the past few years, they have been collected again due to problems.
An insulin spray is absorbed through the oral mucosa, which can be used instead of regular insulin.
New types of insulin
- Lispro: This short-acting insulin function prevents a sudden increase in blood sugar after a meal. This type of insulin can be injected from 15 minutes before eating until shortly after.
- Aspart: This insulin function also regulates blood sugar after a meal, like lispro insulin, but it reaches the peak effect sooner and has a shorter duration of effect.
- Glargine: This type of insulin function is long-acting and slowly absorbed; its level is relatively constant for 24 hours, and once a day injection is sufficient, and it causes less blood sugar drop than other types.
The mentioned types can be used only in exceptional cases and with the attending physician’s opinion.
Inhaled and oral insulins have yet to enter the consumer market.
Features of healthy insulin vials
- The insulin vials you see below are natural and usable.
- A healthy regular (crystal) insulin vial looks completely transparent and uniform.
- An NPH insulin vial appears intact after a gentle shake and palm rolling.
- Signs of unusable insulin vials
- After a gentle shake, the insulin is suspended at the bottom of the vial.
- Insulin looks grainy and has lost some of its smoothness.
- The insulin inside the vial is frozen.
How to store insulin
There are general rules for all medicines, especially for insulin, which include:
Do not expose your insulin vials to extreme cold or heat.
Keep insulin away from direct sunlight. For example, do not put the insulin vial behind the sunny window of your room.
Never put insulin vials in the freezer, refrigerator, etc. Because frozen insulin cannot be used.
Do not place insulin vials near heaters, fireplaces, gas stoves, and air conditioners.
Do not leave your insulin in the closed car during frigid and scorching months of the year.
If you intend to leave the house and the weather is too cold or hot, put your insulin vials in unique thermal insulation bags. You can use small frozen plastic bottles and put your insulin next to them. Ensure that before injecting the insulin, its temperature is the same as the room temperature.
Put the stored insulins in the refrigerator.
Keep the insulins you have opened for your current use at room temperature and away from moisture, cold and heat.
Be careful that the effect of disposable insulin vials whose caps are removed and kept outside the refrigerator will decrease after 28 days.
Injecting cold insulin is painful, so if you keep your used insulin in the refrigerator, take it out of the refrigerator 30 minutes before the injection so that it reaches room temperature.

What points must be observed before injecting insulin?
When buying and using insulin vials, you could pay attention to their expiration date.
Avoid violently shaking the insulin vial because it reduces the effect of the medicine.
Before using insulin, it is necessary to check the insulin vial for the presence of foreign particles and freezing.
Insulin should be clear and uniform until the last drop. If the regular insulin (crystal) inside the vial becomes cloudy, this insulin has lost its effect. The most crucial reason for clouding regular (crystal) insulin is the incorrect order of drawing insulin from the vials (first, you must draw regular insulin into the syringe and then NPH insulin).
After a gentle shake, NPH insulin should be smooth and milky. Otherwise, it cannot be used.
Inject insulin 20-30 minutes before eating.
Observe the injection intervals in one member. The distance between each injection and the previous injection should be 1-1.5 cm.
If you use alcohol cotton, wait until the skin is dry.
If you have drawn a type of insulin into the syringe, you can keep the insulin inside the syringe for up to 1 week in the refrigerator.
Administration and dose of insulin
You cannot take insulin by mouth. This hormone should be injected by syringe, insulin pen, or insulin pump. The type of injection you get depends on your personal preferences, physical needs, and insurance coverage.
Your endocrinologist and metabolism specialist will show you how to inject yourself with this hormone. You can inject this hormone subcutaneously or in different parts of the body, such as:
- thighs
- hip
- upper arm
- belly
Do not inject insulin within a 2-inch radius of your belly button, as the body will not absorb it. You should change the injection site to prevent the thickening of the skin due to repeated injections of this hormone.
Consumption and insulin function differ based on people’s glucose levels and diabetes control goals. Your doctor may instruct you to inject this hormone 60 minutes before each meal. The amount of insulin you need daily depends on factors such as your diet, level of physical activity, and the severity of your diabetes.
Some people only need one dose of insulin per injection. Your doctor may recommend insulin function with immediate or long-term effects.

Insulin function reactions
Hypoglycemia, or deficient blood glucose levels, can sometimes occur when you take this hormone. If you exercise too much or do not eat enough, your blood glucose levels can drop too low and trigger an insulin response. You must balance the amount of insulin you put into your body through food or calories.
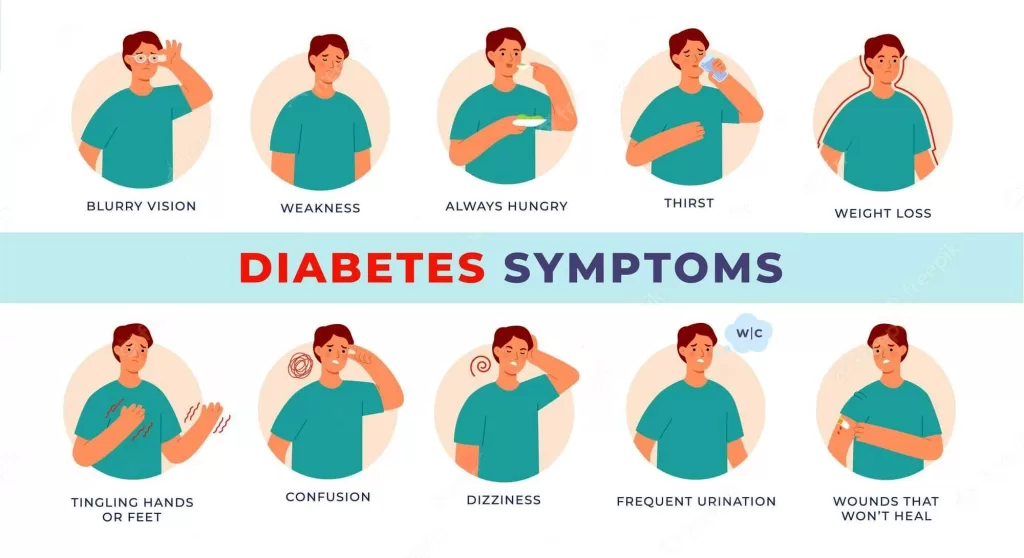
Symptoms of insulin function reaction include:
- tiredness
- Inability to speak
- Sweating
- confusion
- Loss of consciousness
- convulsions
- muscle spasm
- pale skin
Treatment for insulin function
Always carry at least 15 grams of fast-absorbing carbohydrates to prevent an insulin reaction. Including the following:
½ cup non-diet drink
½ cup fruit juice
Five pieces of chocolate
Two spoons of raisins
Ask your doctor about a particular type of pen called a glucagon pen. This pen can help you solve the problem of insulin reaction.
Insulin injection and its side effects
1- Local sensitivity: Redness, swelling, stiffness, or a 2-4 cm protrusion may appear at the injection site within 2-4 hours after injection. This complication usually occurs during the initial stages of treatment. If such a problem occurs, consult your doctor.
2- Widespread sensitivity: this complication is rarely seen, and at first, it happens on the skin and locally, and gradually, it spreads all over the body in the form of hives. Usually, the problem is solved by injecting low insulin doses and gradually increasing it.
3- Insulin lipodystrophy: the local reaction is related to fat tissue, which can be seen in two ways:
- A) Lipoatrophy ß is the loss of subcutaneous fat at the injection site, which can be seen as a shallow or deep depression.
- b) Lipohypertrophy ß The creation of fiber and fat layers at the injection site is caused by repeated use of the same injection site and is seen as a bulge at the injection site.

4- Swelling caused by insulin function, which is the accumulation of more fluids in the organs
5- Insulin resistance
6- Irregular insulin function: which can be seen in two ways: decrease and abnormal increase in blood sugar.
Conclusion
If insulin is used correctly, it will keep your blood glucose level in the correct range. Proper blood glucose levels help reduce the risk of diabetes complications such as blindness and limb numbness. If you have diabetes, monitoring your blood glucose levels regularly is tough.
It would help if you made lifestyle changes to prevent your blood glucose from getting too high. Talk to your doctor about ways to increase the effectiveness of insulin therapy.
Share in :
Explore more


Sitting A Long Time And Being Overweight- Drhealthandbeauty

