

What Are The Risks Factors Of Rhinoplasty?
Table of Contents
Rhinoplasty is a surgical procedure usually performed by an otolaryngologist, maxillofacial surgeon, or plastic surgeon for cosmetic or restorative purposes such as correcting injuries, congenital disabilities, or breathing problems.
Rhinoplasty can be combined with other surgeries, such as eyelid surgery with chin augmentation, to improve cosmetic results.
This surgery has a series of complications, which we discuss in the following article of Drhealthandbeauty and according to the questions of most patients.
The goal of any cosmetic procedure is to improve appearance, not to achieve complete and absolute beauty. Every person applying for this procedure may not be a good option for various reasons; surgery is only recommended for some applicants.
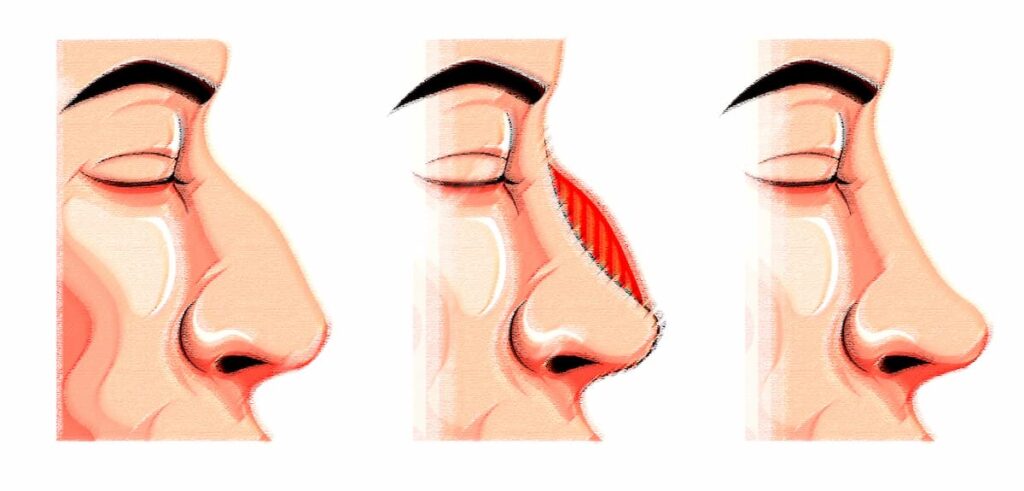
The cause of rhinoplasty dissatisfaction in the fleshy nose
The fleshy nose has thick skin, and the cartilages of the tip of the nose are weak, and the sebaceous glands of the skin of these noses are usually large, and the penetration of these glands into the skin has caused the thickening of the skin.
During the rhinoplasty operation, the surgeon cannot change the skin type and only works on the cartilage and bone of the nose. For this reason, the tip of the nose of those whose noses are fleshy does not shrink much after the operation. It is possible that after the operation, The operated person is unhappy with the tip of his nose not shrinking.
While examining all aspects before the operation, the surgeon will also explain the condition of the person’s skin to the patient.
Suppose you have a massive tip of the nose, and this largeness of the tip of the nose is due to the thickness of the skin. In that case, we are facing the mentioned limitations, but if the size of the tip of the nose is due to the prominent cartilage of the nose, this nose is not fleshy, and there is no problem operating.
If you have doubts about the skin type of your nose and whether it is fleshy or not, I recommend that you visit in person to examine your myopia.

Rhinoplasty is for people who have allergies or wear glasses
Patients with nasal allergies can also undergo surgery. However, these people must be treated with anti-allergic drugs from before the operation until some time after the operation.
Rhinoplasty does not affect vision and eye condition, but since you cannot wear glasses until some time after the operation if you decide to do LASIK, it is better to do eye LASIK first so that you do not need glasses after the nose job.
The presence of orthodontic plaques is not an obstacle for nose surgery and will not cause any problems. Considering that halothane and other inhaled anesthetic gases are used less in private surgery centers today, and new anesthetic drugs either do not have liver effects or, if they do, this effect is small, so if you have had near anesthesia in the past, Not much time must passed since your previous anesthesia.
Rhinoplasty surgery recovery time
Recovery time varies from patient to patient, but the average rhinoplasty recovery time is generally one year.
recovery schedule:
Week 1: The splint will be removed from your nose, and you can go outside with no significant symptoms from the surgery except for bruising around your eye, and it is safe to resume your daily activities.
Week 2: Most of the facial swelling has subsided, and most of the bruises have cleared.
Week 3-4: You can return to your activities, such as running, swimming and cycling
Week 6: The bones have reached a stable state, and you can resume sports training and wear glasses.
3-6 months: Numbness and abnormal sensations in the nose should be resolved.
One year: The healing process is complete – the swelling should have subsided entirely, and the nose’s new shape is visible.
Ways to speed up this table:
- Take a lukewarm shower and avoid heat in the weeks after the operation.
- Avoid doing extreme sports.
- Avoid wearing glasses.
- Stay away from the sun.
- be patient.

Complications and risks of rhinoplasty
Rhinoplasty is associated with many risks because the expectations of the patient and the doctor do not always match. In addition to postoperative abnormalities, many risks and complications are considered.
- These complications and risks include:
Reduction rhinoplasty, for example, can cause breathing problems, which have been reported in 70% of rhinoplasty patients. However, it should be noted that it is the wounds and the loss of mucus that give a person the feeling of a “blocked nose.” give
One of the main risks of autogenous grafts is displacement and resorption, and alloplastic can also cause infection. In this sense, silicone implants with fewer side effects than other materials can have between 5 and 20% side effects.
Skin and soft tissue complications such as numbness, cyst caused by displaced mucus or skin sub-granuloma can be caused by ointment ingredients. Postoperative swelling is mainly due to osteoporosis. Osteoporosis can also cause damage to the orbital region.
Nasal infections are rare, but sometimes they can be dangerous. Osteoporosis can also cause damage to the orbital region. There are reports of other risks, such as brain damage, fistula between the sinus and carotid artery, aneurysm, and cavernous sinus thrombosis. Damaging the veins and nerves makes it possible to change the color of the teeth.
Rhinoplasty abnormalities
Postoperative abnormalities are considered the principal risks of rhinoplasty and cause reoperation in 5% to 15% of cases.
Of course, the analysis of postoperative abnormalities by the doctor allows the identification of specific risks.
Different types of tissues are involved: bone, cartilage, mucosa, skin, fat, fascia, muscles, nerves, and blood vessels, and are not always under the surgeon’s control.
Some “complications” are errors in preoperative analysis or surgical planning, use of inadequate technique, or postoperative care. The severe analysis is essential to prevent this issue.
Abnormalities after Rhinoplasty
Some abnormalities, such as twisted and tense noses, are associated with breathing problems. As a result, 10% of patients complain of breathing problems after rhinoplasty caused by separating the upper lateral cartilage from the septum.

- Abnormalities after rhinoplasty include:
Deep osteoporosis can close the airways in the pyrographic diaphragm, and surgery, removing too much of the cartilage of the alar, causes the collapse of the alar and semicircular wounds. However, rhinoplasty is not possible for bad breathing performance.
If the nose is blocked, it should be inspected or measured, and loss of mucosal sensitivity should be noted. The sensation of hot and cold air during breathing is essential for perception through the nose.
Loss of sensitivity due to surgical wounds can cause the sensation of blocked nasal airways.
Additional surgical interventions, such as combinations on the turbinate or enlargement of the nasal vestibule, worsen the situation.
Hyposmia after rhinoplasty is only temporary in most cases due to mucosa swelling. It can only be found by testing and not even realized by the patient.

Risks of nose transplants and implants
The main risks for implantation and grafting in the nose include infection, extrusion, rejection, and resorption, and these complications occur in less than 1%. Among 184 cases, only eight twisted or twisted autogenous costal cartilages were found.
In addition to five displaced implants and silicone, autogenous rib cartilage is only needed for augmentation in primary rhinoplasty. With good technique, the risks for absorption and distortion are minimal, even in long-term follow-up.
Depending on the absorption conditions of the recipient area, the use of autogenous cartilage is a problem. Due to the large surface area compared to solid cartilage, significant absorption should be expected with dense cartilage.
It is possible to support the survival of blood cells by wrapping the cartilage with lata fascia; on the other hand, even the unwanted growth of the cartilage is possible.
Causes of bruised eyes after Rhinoplasty
Eye bruising after rhinoplasty is a completely normal issue, and do not forget that rhinoplasty, both open and closed, is one of the most invasive cosmetic surgeries. Because the patient’s face bears much pressure during the surgery, it causes bruising and inflammation later. From surgery, it is an expected issue.
During rhinoplasty surgery to treat breathing problems or to create a new shape in the nose, the surgeon is sometimes forced to break the nasal bone so that the shape can change quickly; this causes swelling and bruising in the eye, nose and cheek area.
Several factors affect the severity of eye bruising. For example, the age of people is one of the critical factors in this matter.
Usually, the blood vessels in the periosteum are weaker and more vulnerable in people over 45. Therefore, it is normal for people over 45 to experience more severe bruising.
Factors affecting eye bruising after rhinoplasty are generally divided into personal and surgeon-related factors.

Essential factors in aggravating eye bruises
These factors include:
If the nose is broken before surgery (osteotomy surgery) or is broken during rhinoplasty.
Use of open nose surgery technique.
The amount of cut that needs to be made in the periosteum layer.
The patient’s age and the skin’s thickness (the thinner the skin, the more quickly it shows the clotted blood vessels.)
Bad smell after rhinoplasty
Nasal odor is due to infection after nose surgery and may cause bad breath. This complication can occur in the first two weeks to one month after nose surgery.
A foul smell in the nose is not a sign of a particular problem and is nothing to worry about. The cause of this complication may be the presence of blood clots left over from the surgery.
To solve this problem, consult your surgeon and wash the inside of the nose.

Nasal infection after rhinoplasty
After rhinoplasty, there is a possibility of infection. This infection slows down the healing process of the scar and even affects the results of nose surgery.
- Aggravating factors of nasal infection include:
Ingress of contamination, such as water contaminated with microbes
Not paying attention to personal hygiene and cleanliness of the environment
Non-sterility of the surgical environment and its equipment
The recovery period of rhinoplasty
You can go home immediately after rhinoplasty. The bruising and swelling of your face will decrease every day. Remember, due to the thinness of the skin, the swelling on the bridge and upper parts of the nose will go away faster.
The swelling of the tip of your nose will take longer to go down as the skin in this area is thicker. If your nose is deviated, the bruising and swelling of your nose will disappear later.
During the first 24 hours after the procedure, you may feel sleepy. This is one of the side effects of anesthetics! Do not forget that you should not drive after receiving anesthetic drugs.
For the first 24 hours after the operation, you should stay home, do nothing and rest. Early nose care after surgery is critical to speeding up recovery time. You should use cold water compresses to reduce swelling and bruising.
The first night, you should sleep completely flat; use two to three pillows to drain your nose and reduce swelling and bruising.
Conclusion
In short, the reasons for changing the nose’s size, the nose’s angle, straightening the nose’s bridge, shrinking the nostrils, and changing the shape of the tip of the nose can be called rhinoplasty.
If the operation aims to bridge the nose, the surgeon will remove the bone and cartilage that caused the hump. After that, it brings the rest of the bone pieces together and narrows the nose. For nasal tip surgery, the cartilage of this area is removed through a small incision in the middle of the nose (called the columella). The surgeon can change the central structure of the nose by cutting and adjusting the cartilage, and it also helps to reduce the length of the nose.
If this surgery is not performed by a specialist doctor, in addition to the inappropriate shape of the nose, it may also hurt the sense of smell and breathing.
All surgeries have risks, such as infection, bleeding, or a bad reaction to anesthesia.
Rhinoplasty may increase the risk of breathing problems, nosebleeds, nasal numbness, asymmetric nose, and wound.
References”
Share in :
Explore more


Sitting A Long Time And Being Overweight- Drhealthandbeauty

